Cómo tratar las úlceras por presión severas y recuperar la salud
Title: How to Treat Severe Pressure Ulcers and Restore Health Profile: Pressure ulcers require personalized treatment and prevention. Combined methods are highlighted to accelerate healing. Keywords: ['Medical Care', 'Chronic Diseases'] Author: Yao Yao, Department of Bone Injuries, Hunan Province Integrative Traditional and Western Medicine Hospital (Affiliated Hospital of Hunan Academy of Traditional Chinese Medicine) Reviewer: Chen Xilong, Director of the Bone and Joint Injuries Section Commissioner: Chen Yansheng, Deputy Chief Physician of the Bone Injuries Department Production Information: Hunan Province Integrative Traditional and Western Medicine Hospital, Hunan Province Academy of Traditional Chinese Medicine.
In daily life, groups with limited mobility, such as bedridden elderly individuals, patients with paraplegia, and those undergoing surgery who remain still for extended periods, are prone to developing pressure ulcers (commonly known as "bedsores") due to prolonged pressure on local tissues and compromised blood circulation.
This type of skin damage gradually progresses from initial erythema to deep ulcers. Severe pressure injuries (stage IV) affect muscles and bones, with recurrent pus presence, and can induce sepsis and multiple organ failure. When combined with underlying diseases, the mortality rate remains high, making it a "persistent problem" that is difficult to manage in care settings.
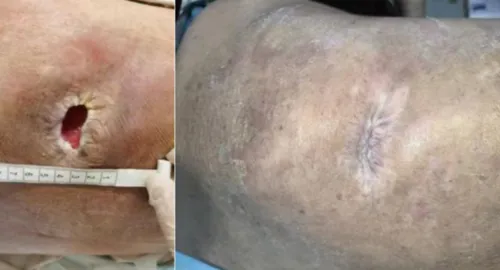
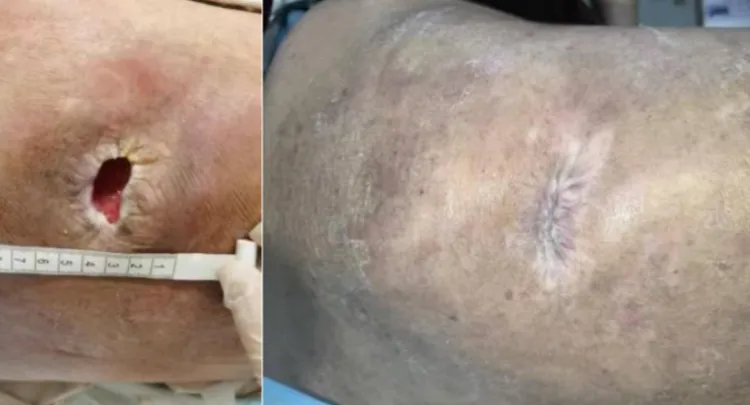
Elder Qin, 78, is a victim of severe pressure ulcers. Due to prolonged bed rest and feeding through a nasal tube, he presents two suppurating lesions on his back and sacral region, with bone exposure, accompanied by symptoms such as mental weakness and difficulty breathing.
After evaluation at a local hospital, the family was informed that the elderly patient, in fragile condition, also exhibited hypoalbuminemia and lung infection, indicating a long treatment period and high risks. Through the recommendation of other patients, Qin's family arrived at the Fourth Section of Traumatology of the Hunan Province Integrative Traditional and Western Medicine Hospital (Affiliated Hospital of Hunan Academy of Traditional Chinese Medicine) for medical care.
Precision in breaking: individualized approach combining Chinese and Western medicine + Negative Pressure Wound Therapy (NPWT).
Dr. Chen Yansheng, Deputy Chief Physician of the Bone Injuries Department, after conducting a wound assessment, laboratory tests, and diagnostic imaging, confirmed that Mr. Qin has a stage IV pressure ulcer (infected type), alongside hypoalbuminemia that has led to a deficiency in the "materials" necessary for tissue repair. The lung infection has exacerbated the overall inflammatory response, creating a vicious cycle among the three factors. In light of this complex situation, the team designed an individualized plan consisting of "infection control + nutrition + repair."
1. NPWT: utilizes negative pressure suction technology to continuously remove infectious secretions from the wound, eliminate necrotic tissue, and block the spread of infections, creating a "clean environment" for wound healing.
2. Adjustment of Traditional Chinese Medicine treatment for underlying diseases: for hypoalbuminemia, herbal formulas are used to strengthen the spleen and increase energy, as well as nourish the blood and correct deficiencies, complemented by carefully balanced enteral nutrition providing high-quality proteins and trace elements, thus improving the body's nutritional status. In cases of lung infections, herbal formulas are applied to disperse lung qi, eliminate phlegm, and clear heat and detoxify, along with moxibustion on specific points to reduce lung inflammation and relieve respiratory discomfort.
3. External treatment of Traditional Chinese Medicine to promote recovery: in the postoperative phase, external applications of Chinese herbs and smoke baths are used to reduce swelling and pain, activate blood circulation, and stimulate the growth of granulation tissue.
After a month of systematic treatment, Elder Qin's two severe pressure ulcers completely healed, his skin returned to smoothness, and symptoms of hypoalbuminemia and lung infection significantly improved, with difficulty breathing and mental lethargy entirely gone. In a non-oxygen state, blood oxygen saturation stabilized at over 95%, leading to a successful rehabilitation discharge.
(▲ Back)
(▲ Sacrococcygeal region)
Recognition of pressure ulcers: key knowledge from staging to diagnosis.
1. Stage I: Redness of the skin that does not fade when pressed. The skin may feel warm or cool to the touch, and the texture may change compared to the surrounding skin. 2. Stage II: Partial loss of skin thickness, which may appear as a blister, abrasion, or superficial ulcer. The base of the wound may be a pink-red color. 3. Stage III: Total loss of skin thickness, which may extend to the dermis and underlying tissues. The wound may present necrosis of adipose tissue, but it does not involve muscle or bone. 4. Stage IV: Total loss of skin thickness with extensive tissue destruction, which may include exposed muscles, tendons, or bones. Signs of infection may be present, and immediate medical attention is necessary.
Stage I: The skin is intact and presents red spots that do not disappear upon pressing, being this a crucial period for preventive intervention.
Stage II: Loss of epidermis, formation of superficial ulcers, requiring timely wound cleaning and skin protection.
3. Stage III: The ulcer extends into the subcutaneous tissue, with visible adipose tissue, and requires specialized care intervention.
Stage IV: The lesion profoundly affects muscles and bones, accompanied by necrotic tissue and severe infection, classified as a severe pressure ulcer and requiring comprehensive treatment.
Two or three steps for accurate diagnosis.
1. Wound assessment: Medical personnel evaluate the ulcer stage, depth, and degree of infection through visual examination, palpation, and measurement.
2. CT/MRI evaluation: clearly shows the extent of necrosis in underlying tissue and possible osteomyelitis, providing an accurate basis for treatment.
3. Laboratory tests: Assess nutritional status, infection indicators to guide nutritional support and antibacterial treatment.
Prevention of pressure ulcers: "Skin care program" for long-term bedridden individuals.
In conjunction with Elder Qin's case of pressure ulcer due to prolonged bed rest, caregivers can take the following actionable preventive measures for high-risk populations: 1. Regularly change positions: change the patient's position every two hours to relieve pressure on the skin. 2. Use suitable mattresses: choose pressure-relieving mattresses, such as air mattresses, to help distribute weight and reduce the occurrence of pressure ulcers. 3. Keep skin dry and clean: regularly wash the patient's skin to ensure it remains dry, preventing moisture-related skin damage. 4. Increase nutritional intake: ensure the patient receives adequate nutrition, especially proteins, vitamins, and minerals, to promote skin healing. 5. Regularly check skin condition: caregivers should regularly check the patient's skin, particularly pressure points, to detect and address issues early. 6. Engage in moderate exercise: encourage patients to perform appropriate activities and exercises to promote blood circulation. Through these measures, the risk of pressure ulcers can be effectively reduced for high-risk populations.
1. Regularly turn the patient: Help the patient turn every 2 hours to avoid continuous pressure on local tissues. When turning, perform movements gently to avoid dragging or rubbing the skin.
2. Optimize positioning: use auxiliary tools such as air mattresses and pressure-relieving pads to disperse pressure on bony prominences (such as the sacrococcygeal area, back, and heels) and maintain limbs in a functional position.
3. Skin care: Clean the skin daily with lukewarm water, keep the skin dry and clean, avoid irritants such as sweat and urine, and choose loose, breathable cotton clothing.
4. Nutritional support: for patients receiving tube feeding or having difficulty eating, it is crucial to ensure intake of high-quality proteins (eggs, milk, fish, meat, etc.), as well as vitamins and trace elements, to prevent hypoalbuminemia.
5. Early observations: Review the skin condition daily. If red spots that do not fade upon pressing (stage I pressure ulcer) are detected, decompression measures should be taken immediately to prevent the condition from worsening.
Experts warn.
Director Chen Xilong of the Bone and Joint Injuries Section warns that the core of preventing and treating pressure ulcers is "early prevention, early detection, and early treatment." Caregivers for high-risk individuals should pay attention to daily care, implementing measures such as position changes, pressure reduction, and skin care. If redness or skin damage is detected, intervention should be timely.
If a pressure ulcer has already formed, the wound should not be managed independently, especially in patients with underlying diseases. It is necessary to seek care from a specialized hospital, where an individualized plan combining traditional and Western medicine is implemented, taking into account both wound repair and treatment of the underlying disease. At the same time, nutritional support and daily care are important guarantees for successful treatment. The collaboration of these three elements can improve efficacy and reduce the risk of complications.
Hunan Medical Chat Special Contributor: Yao Yao, Four Departments of Bone Injuries (Trauma Surgery) of Hunan Province Integrative Traditional and Western Medicine Hospital (Affiliated Hospital of Hunan Academy of Traditional Chinese Medicine)
© 2025 Tribu Salud.