4 causas de picazón y engrosamiento en la piel que debes conocer
Title: 4 Causes of Itching and Thickening of the Skin You Should Know Author: Unknown Reviewer: Unknown Commissioner: Unknown Production/Organization: Unknown Profile: Nervous dermatitis is a chronic skin disease that causes itching and thickening of the skin. Keywords: ['Skin Health', 'Mental Health']
Suddenly, intense itching begins on the eyes, temples, neck, waist, elbows, and other parts of the body, making it hard to resist scratching and difficult to stop.
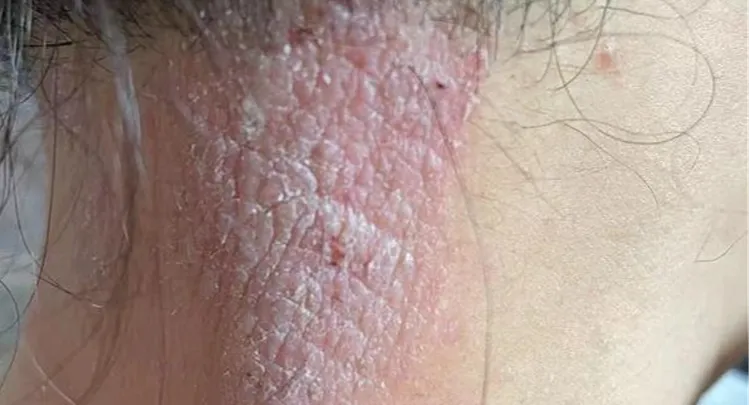
Shortly after, the skin becomes rough and thick, the skin tone darkens and reddens, resembling ringworm; this could be a sign that nervous dermatitis has made its appearance.
Neurodermatitis, also known as chronic simple lichen, is a common chronic skin disease characterized mainly by intense itching of the skin and lichen-like changes.
Its most typical feature is the cycle of 'the more you scratch, the itchier it gets, and the itchier it gets, the more you scratch,' leading to difficulty in liberation once entangled.
Its process of exacerbation is divided into three steps:
Initiation of provocation: an inexplicable itch appears on some part of the skin, causing one to scratch uncontrollably.
Starting a cycle: once scratching begins, the sensation intensifies, leading to more intense and frequent scratching unconsciously.
Leaving marks: prolonged repeated scratching and friction lead to skin thickening, becoming rough, dry, and flaky, ultimately forming lichen-like plaques.
What is even more torturous is that it severely affects quality of life. Daytime itching is bothersome, and nighttime outbreaks interrupt sleep, causing insomnia and anxiety... it is truly disturbing!
The cause of neurogenic dermatitis is quite complex, but the medical community currently considers it closely related to the following three main factors.
1. Great mental pressure (main cause)
Prolonged nervous tension, excessive stress, anxiety, or lack of sleep can affect the normal regulatory function of the nervous system, potentially causing or worsening skin itching. Many patients report that during periods of emotional changes or intense stress, symptoms tend to intensify.
2. External stimuli and friction.
Localized friction on the skin is another common factor. For example, repeated friction in areas like the neck or belt, the use of inappropriate clothing materials, or constant scratching following mosquito bites can be external stimuli that directly induce neurogenic dermatitis.
3. The influence of lifestyle habits.
Certain lifestyle habits or physical conditions may influence the disease, such as alcohol consumption, intake of spicy foods, or the presence of gastrointestinal and endocrine disorders, which could become potential factors that trigger or exacerbate symptoms.
Neurogenic dermatitis is mainly divided into two types: localized and disseminated.
Limited neurogenic dermatitis is common in areas such as the neck, elbows, and eyelids.
The location of the lesion is quite localized, typically featuring only one skin lesion, with a diameter of approximately 2 to 6 centimeters, well-defined edges, a mildly scaly surface, and its color is similar to normal skin tone or slightly darker.
Due to constant scratching, the affected skin often shows scratch marks and bloody scabs around. Repeated scratching may stimulate skin thickening, causing a lichen-like transformation.
● Diffuse neurodermatitis, with a broader distribution range, often affects the head, extremities, and trunk.
Symptoms are similar to localized types, characterized by paroxysmal severe itching, especially worsening at night, severely affecting sleep.
Frequent scratching may break the skin, which not only exacerbates existing skin issues but also promotes skin infections, forming a vicious cycle.
The treatment of neurogenic dermatitis includes the following aspects:
It is important to maintain a good mood, rest adequately, follow a light diet, avoid anxiety and tension, try to refrain from staying up late, and keep a regular schedule.
② Strengthen hydration and local moisturizing, and reduce stimuli such as scratching.
A topical corticosteroid or calcineurin inhibitor ointment can be applied to the affected area.
For severe cases, oral antihistamines are recommended.
However, neurogenic dermatitis presents symptoms that are quite similar to those of other skin diseases such as eczema, psoriasis, and atopic dermatitis, making it difficult for common people to accurately differentiate them. Therefore, before using any medication, remember to consult a specialized doctor for an accurate diagnosis!
© 2025 Tribu Salud.