Cómo cuidar el pie con arteriosclerosis obliterante en las extremidades
Title: How to Care for Feet with Obliterative Arteriosclerosis in the Extremities Author: Yang Xiaoling, Nurse in the Vascular Surgery Department of Xuanwu Hospital, Capital Medical University. Reviewer: Wu Rui, Deputy Chief Nurse of the Vascular Surgery Department of Xuanwu Hospital, Beijing Medical University. Production: Popular Science China Profile: Arterial occlusion in the legs can cause foot ulcers. Daily care and proper measures can reduce risks.
Foot ulcers caused by peripheral arterial obstructive disease are mainly due to a severe narrowing or blockage of blood vessels in the legs, resulting in ischemia and prolonged oxygen deprivation in the feet. To illustrate this more clearly, it is as if the 'blood supply channels' of the leg are rusted and blocked, preventing the distal tissues from receiving enough blood for nourishment, naturally making the foot weaker. In this situation, even a small insignificant wound can evolve into a hard-to-heal ulcer due to the lack of necessary nutrients and oxygen for repair, and in the most severe cases, there is a risk of amputation.
Therefore, for patients and their families, foot care is not simply about 'washing feet frequently'; it is a key part of delaying disease progression and preserving limbs. We will approach the topic from the standpoint of 'why ulcers are easily developed,' clarifying the reasons and gradually mastering scientific and practical daily care methods to genuinely protect our feet.
The reasons why patients with lower limb arteriosclerosis are prone to foot ulcers are mainly as follows: 1. Poor blood circulation: Arteriosclerosis leads to narrowing and reduced elasticity of blood vessels, hindering blood flow and thus reducing blood supply to the lower limbs, especially the feet. This ischemic state makes foot tissues more susceptible to damage, leading to ulcer formation. 2. Nerve dysfunction: Arteriosclerosis is often accompanied by diseases such as diabetes, which can lead to sensory nerve damage, diminishing patients' ability to perceive foot injuries and pressure, making them prone to neglect small wounds that can develop into ulcers. 3. Poor foot environment: Due to insufficient blood supply and missing nerve sensations, patients may experience dry, cracked skin on their feet, increasing the risk of ulcer occurrence. 4. Increased infection risk: Insufficient blood flow to the feet reduces the efficiency of immune responses, making it easier for ulcers, once formed, to become infected and worsen the condition. 5. Impact of underlying diseases: Many patients with lower limb arteriosclerosis also have other chronic diseases like diabetes or hypertension, which increase the risk of foot ulcers due to their presence. In summary, patients with lower limb arteriosclerosis are more likely to develop foot ulcers due to a combination of factors such as poor blood circulation, nerve injury, a poor foot environment, and the risk of infection.
1. Root cause: The severe ischemia in the foot caused by arteriosclerosis results in narrowing or blockage of blood vessels in the legs. The foot, being the farthest part, suffers from a severe lack of blood supply. Tissues in prolonged hypoxia become fragile; once injured, they have great difficulty healing due to a lack of nutrients, ultimately resulting in the formation of ulcers.
2. Increased suffering: Underlying systemic diseases such as diabetes damage nerves and blood vessels, causing loss of sensitivity in the feet, making injuries hard to notice and extremely difficult to heal; hypertension accelerates thickening and sclerosis of vessel walls, aggravating ischemia in the lower extremities; hyperlipidemia promotes the formation of atheromatous plaques, narrowing the lumen; chronic renal failure causes alterations in calcium and phosphorus metabolism leading to vascular calcification and worsening distal ischemia; heart failure or arrhythmias reduce cardiac output, decreasing perfusion pressure in the extremities and exacerbating ischemia.
3. Direct triggering factors: local physical and mechanical factors. Most ulcers do not occur spontaneously but are provoked by everyday details. Foot deformities (claw toes, hammer toes, etc.) cause abnormal friction points with footwear; calluses compress deep soft tissues, which may result in internal necrosis; wearing inappropriate footwear that is too tight or contains foreign objects can cause skin erosions; trauma: improper nail cutting, burns (from hot water bags, heaters), frostbite, or wounds from walking barefoot; fungal infections (athlete's foot) cause cracks and erosions in the skin, opening the door to bacterial invasion.
4. Infection factors: catalysts for wound deterioration. Once the skin barrier is broken, due to poor local blood circulation, white blood cells and antibiotics have difficulty reaching the area, which can cause mild cellulitis to progress rapidly to osteomyelitis or gangrene.
5. Poor habits and procrastination can also have negative effects. Smoking causes significant damage to blood vessels as it leads to their contraction and aggravates ischemia. Some people think that having cold feet or experiencing leg pain after walking a short distance is a normal aging phenomenon and do not consult a doctor, which can lead to severe consequences. Others may have poor vision and cannot see if they have small wounds on their feet, or they may not follow medical advice in taking their medications, worsening their condition.
Key points for daily foot care: how to scientifically care for the feet?
1. Choose suitable shoes and socks. Use round-toed, wide, and breathable shoes, avoiding pointed and hard-soled footwear. Wear cotton socks that do not constrict the ankles. Before putting on shoes, check for foreign objects inside. Never walk barefoot to prevent cuts.
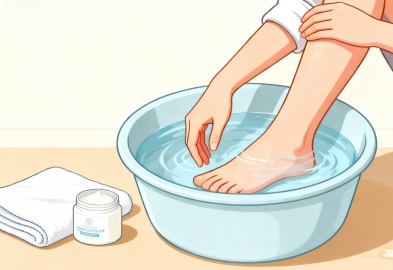
2. The water temperature for foot baths should be maintained between 37 °C and 39 °C (test the temperature with your elbow), soaking for 10 to 15 minutes. Use a soft towel to gently dry the feet, and make sure to dry well between the toes. If the skin is dry, you may apply moisturizer, but avoid areas with cuts.
3. Trim toenails. After soaking the feet, trim the nails while they are softer, making it easier to avoid breakage. Cut the nails straight, level with the fingertips, without leaving them too short or rounded. After cutting, smooth the edges. Calluses and bunions should be treated by a doctor.
4. Keep warm; in cold weather, wear thick socks to retain heat. It is strictly prohibited to use hot water bags, foot warmers, or electric blankets to heat the feet directly, as the lack of blood supply can lead to decreased sensitivity in the feet, making them very prone to burns.
5. To prevent bumps, walk slowly to avoid collisions. When sitting, avoid crossing legs to prevent compressing blood vessels. Legs can be slightly elevated to promote venous return. Control body weight to reduce pressure on your feet.
6. Manage chronic diseases well. If you suffer from hypertension, diabetes, hyperlipidemia, etc., make sure to take medication on time and undergo regular check-ups, keeping values within normal ranges.
7. Perform daily self-evaluations and seek medical attention if there are any problems. Each night, examine your feet: look for signs of redness, ulcers, or blisters; touch to check the skin temperature and ensure the pulse of the dorsal arteries of the foot is normal.
Foot health is fundamental to walking and living normally. Attention to daily details is necessary to distance ourselves from the risk of ulcers and take care of our feet.
© 2025 Tribu Salud.

