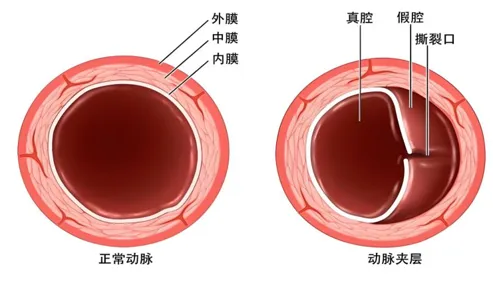
No cepillarse bien los dientes puede favorecer el cáncer: descubre por qué
Title: Poor Tooth Brushing Can Promote Cancer: Discover Why Author: Jiang Yongyuan, Master in Internal Medicine, Third Military Medical University Reviewer: Pan Zhanhe, Chief Physician, Department of Oncology, Zhongshan University Hospital, and Vice President of the Professional Cancer Disclosure Committee, Fujian Cancer Association. Planning: He Yumeng Editor: He Yuming Reviewers: Xu Lai, Zhang Linlin Source: Official WeChat of Popular Science in China The cover image of this article and the images within the text are sourced from a copyright image library. Reprinting may lead to copyright disputes.
Who would have imagined that not brushing one’s teeth properly could facilitate the metastasis of cancerous cells. In December 2025, a research team from Wuhan University published a study that garnered significant attention. They discovered that a common periodontal pathogenic bacterium, called Porphyromonas gingivalis, could influence the metastasis process of esophageal squamous cell carcinoma by releasing small "vesicles" [1].
In summary, this study reveals a possible biological mechanism: bacterial products from the oral cavity could facilitate the spread of cancerous cells through a series of changes in intracellular signaling.
However, before jumping to conclusions, it is necessary to put the facts back into a scientific context to understand what these studies really tell us and what they do not.
From "oral bacteria" to "tumor metastasis." The evidence continues to accumulate.
The research from Wuhan University found for the first time that the abundance of Porphyromonas gingivalis in esophageal squamous cell carcinoma tissue is significantly higher than in adjacent normal tissue. Additionally, as the abundance of this bacterium increases, patients tend to have more advanced stages of disease, more lymph node metastases, and lower survival rates. Further experiments on cells and animals demonstrated that extracellular vesicles released by this bacterium can enhance the migration and invasion capacity of tumor cells, thereby facilitating the emergence of metastases.
The schematic diagram illustrating the mechanism by which Porphyromonas gingivalis exosomes promote the progression of esophageal squamous cell carcinoma | Reference [1]
This is not an isolated finding. Another study based on transcriptome data showed that infection with Porphyromonas gingivalis significantly alters the expression profile of inflammation-related genes in esophageal squamous carcinoma cells, and patients with significant infection-related gene characteristics had a shorter overall survival time [2].
According to the expression level of genetic characteristics associated with Porphyromonas gingivalis infection (A-C), researchers categorized patients into a high expression group and a low expression group, comparing overall survival between both groups (Kaplan-Meier survival curve) | Reference [2].
These studies molecularly support the notion that chronic oral infections can, through inflammation and signaling pathways, remodel the tumor microenvironment, thus affecting disease progression.
Epidemiological research also supports this conclusion.
A retrospective study compared 60 esophageal squamous carcinoma patients to 178 healthy controls and found that individuals with more severe periodontal attachment loss and more missing teeth had a higher proportion among esophageal carcinoma patients. Moreover, in patients undergoing radical surgery for esophageal cancer, those with moderate to severe periodontal inflammation preoperatively had significantly worse long-term survival compared to patients with good periodontal status.
The association between periodontitis in post-esophagectomy patients (with or without periodontitis) and overall survival (OS) (A) and disease-specific survival (DSS) (B) | Reference [4]
Similar associations have been observed in other regions and in other types of digestive tumors. A large case-control study in the Kashmir region showed that, compared to individuals who never clean their teeth, the proportion of patients with esophageal squamous carcinoma was significantly lower in the population that cleans their teeth at least occasionally. Conversely, in a nested case-control study in southwest China, the proportion of esophageal and colorectal cancer in the population with periodontitis was approximately double that of those without periodontitis, and additionally, in some tumor types, it was also related to higher rates of metastasis.
Correlation does not imply causation.
How should we understand these findings?
Seeing these results, many people might instinctively ask: Does having periodontal disease necessarily lead to digestive tract tumors? The answer is no.
Existing studies mostly suggest correlation rather than definite causation. Periodontal disease often coexists with factors like smoking, alcohol consumption, dietary habits, and socioeconomic status, all of which are significant factors influencing digestive tract tumors. Even when adjustments are made in statistical analyses, it is impossible to completely isolate the effects of all confounding factors.
Compared to individuals who never clean their teeth, the proportion of patients with esophageal squamous carcinoma among at least occasional tooth cleaners is markedly lower.
Moreover, there is a significant gap between mechanistic research and the real world. The study from Wuhan University provides us with a clear molecular explanation framework, but this does not necessarily mean that in the general population, Porphyromonas gingivalis drives tumor occurrence through the same pathway. In many cases, it may only be involved in a network of chronic inflammation, rather than being a single switch.
Thus, a more reasonable understanding is that periodontal diseases may be a risk factor associated with the occurrence and progression of tumors in the digestive tract, rather than a decisive factor in the outcome.
Let us not induce panic, but neither should we ignore it.
Ordinary people can do many things. Firstly, they can dedicate their time and effort to help others, such as participating in volunteer activities or supporting local community projects. Secondly, ordinary people can enhance themselves by learning new skills and knowledge, pursuing personal and professional development. Additionally, they can actively engage in social activities, express their views, and influence policies and decisions. Lastly, ordinary people can spread positive energy through daily acts of kindness, bringing positive change to society.
These researches remind us that oral health is closely related to other organs in the body, and that a state of persistent inflammation can affect overall health in various ways.
For most people, this does not mean frequent screening for tumors, nor does it mean that the discovery of periodontal issues immediately implies cancer. What is truly meaningful is to incorporate oral health into daily health management.
The regular practice of dental brushing, the use of dental floss, and the reduction of chronic gingivitis and periodontal infections can improve quality of life and, in the long term, decrease the burden of chronic inflammation.
What truly matters is to incorporate oral health into daily health management.
For patients already diagnosed with digestive tract tumors, these studies provide a clinically significant detail. Multiple studies have shown that preoperative or pre-treatment standardized oral assessment and management are correlated with better prognosis. However, this does not mean that "treating dental issues can cure cancer," but rather that by reducing the burden of infections and inflammation, the body is in a more favorable condition during treatment.
The value of science lies in helping us make more rational decisions. The relationship between periodontal diseases and digestive tract tumors is gradually being delineated, and what we can do remains the most basic and safe: to consider daily oral cleaning as a long-term investment in our health.
References
Hong K, Zhang H, Qi J, et al. The extracellular vesicles of Porphyromonas gingivalis promote tumor metastasis in esophageal squamous carcinoma by inducing the PRKACB/JNK/NFATC2 axis. J Nanobiotechnology. 2026;24:66.
Kong J, Liu Y, Wang J, et al. A new genetic signature of inflammatory response related to Porphyromonas gingivalis infection predicts prognosis in esophageal squamous cell carcinoma. Clin Med Insights Oncol. 2024;18:1–15.
Haque T, Nabhan AB, Akhter F, et al. The analysis of periodontal diseases and esophageal squamous cell cancer: a retrospective study. Saud. Dent. J. 2023;35:714-719.
Nozaki S, Sato Y, Takano H, et al. Pre-treatment periodontitis is a predictor of worse prognosis after esophagectomy for esophageal cancer. Esophagus. 2024;21:120–130.
Dar NA, Islami F, Bhat GA, et al. Poor oral hygiene and risk of esophageal squamous cell carcinoma in Kashmir. Br J Cancer. 2013;109:1367–1372.
Luo T, Li J, Pu K, Yang G. Association between periodontitis and the risk and prognosis of gastrointestinal cancer: evidence from a nested case-control study in southwest China. Eur J Med Res. 2025;30:225.
Planning and production.
© 2025 Tribu Salud.